Introduction
The concept of iv drip chamber is central to safe intravenous therapy and medical device management. Healthcare providers who understand this subject deliver better, safer care to patients in hospitals, clinics, and home health environments.
Understanding the Fundamentals
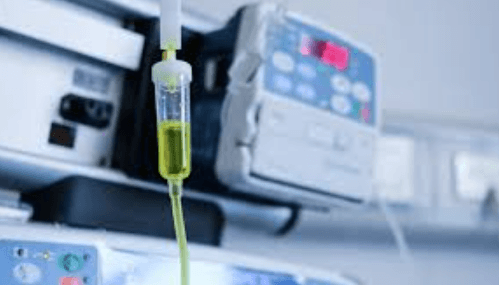
An IV set is a sterile, single-use medical device designed to transfer fluids from a bag or bottle directly into a patient’s vein. Its components are carefully engineered to prevent contamination, air entry, and fluid leakage during administration.
Spike Adaptor and Its Function
The spike adaptor is the piercing device at the top of the IV set. Its pointed tip is designed to puncture the rubber port of an IV bag. Some versions include air-vent ports for use with glass bottles, allowing air displacement as fluid flows out continuously.
IV Tubing and Connection Ports
The main tubing connects all components from the fluid bag to the patient’s access point. Connectors along the line allow for secondary infusions or medication additions. High-quality tubing is kink-resistant and manufactured from medical-grade PVC that is compatible with most IV solutions.
Clinical Best Practices
When considering iv drip chamber in clinical practice, it is important to follow evidence-based guidelines and institutional protocols.
Depending on clinical applications, IV sets may include additional components such as bacterial filters, burette chambers for pediatric dosing, or photosensitive coverings for light-sensitive medications. These specialty parts significantly expand the functionality of standard IV sets.
- Select the appropriate equipment based on patient age and clinical indication
- Ensure compatibility between the device and the prescribed medication
- Prime the IV line thoroughly to remove all air before patient connection
- Secure all connections to prevent accidental disconnection during care
- Label the IV line clearly with date, time, and rate information
Common Challenges and Solutions
All parts of an IV set must remain sterile during priming and administration. Clinicians should use aseptic technique, avoid touching sterile surfaces, and change IV sets per hospital protocols typically every 72 to 96 hours.
See also: Common Health Considerations for Labradoodles
Frequently Asked Questions
FAQ 1: What regulatory standards govern this type of medical equipment?
IV therapy equipment is governed by international standards including ISO 8536 for infusion equipment and ISO 10993 for biocompatibility of medical devices. National regulatory bodies like the FDA also oversee product approval and market surveillance.
FAQ 2: How can clinicians reduce errors related to this topic?
Error reduction strategies include standardized protocols, regular staff training, double-checking calculations and connections, using color-coded systems, and applying barcode medication verification where available.
FAQ 3: What is the proper technique for handling these medical supplies?
All intravenous supplies must be handled with clean or gloved hands using aseptic non-touch technique. Maintain sterility at all times, avoid touching critical connection points, and inspect packaging integrity before use.
Conclusion
Mastering iv drip chamber empowers clinicians to work with greater confidence and precision. The information presented here reflects current best practices and supports the delivery of high-quality intravenous therapy across all clinical environments.